23.6 Million Have This Disease. 5.4 Million Do Not Know They Have It!
Diabetes is a chronic, crippling disease that is debilitating both our older and younger generations in record numbers. Fully 20% of all hospital admissions and doctors' office visits are for patients who suffer from diabetes, many of whom do not even know they have the disease.
In the United States, 1 in 20 individuals suffer from diabetes. The incidence of diabetes is rising rapidly in the US at a rate of 6% per year and currently is the seventh leading cause of death. At this rate of increase, the number of people in the US who suffer from diabetes will double every 15 years. However, other than the fact that people with diabetes have a lack of insulin, what else do we know? Are you aware that Diabetes Mellitus (DM) is the most common type of metabolic disease of humans and is strongly associated with Western culture and diet, perhaps more strongly than any other disease process. Did you know that most symptoms and health problems associated with diabetes are actually not from the lack of insulin, but are from complications of the disease, which include nerve disorders, blindness, very accelerated
hardening of the arteries, cataracts, impaired circulation and gangrene which can lead to the amputation of limbs?
The Disease
So, what is diabetes? A little explanation of cellular physiology is in order here. The cells in our bodies use carbohydrate for energy. This carbohydrate is usually provided to the cells in the form of glucose. When we consume a meal, it is broken down in our digestive system. The nutrients, including glucose, are absorbed and carried in the bloodstream throughout the body to feed each cell. But our individual cells are locked up tight and do not freely allow molecules to pass in and out of them. Their cellular environments must be tightly controlled or they would die. Therefore we need something to act as a key to open the door to our cells so that they can eat the glucose that has been delivered to them. That’s where insulin comes in. Insulin is a hormone made in specialized cells of the pancreas called the beta cells of the Islets of Langerhans. Insulin acts like a key, or a gatekeeper opening the locks to the cells, and assists glucose to enter the cells so that our cells can eat. Diabetes is a lack or absence of insulin or it is an inability to use the insulin that is produced. For various reasons, the body either stops producing insulin, or our cells no longer recognize the insulin and the insulin key no longer fits the locks of the cells. In either case, we find that the level of glucose builds up to very high levels in the blood, a condition referred to as hyperglycemia, while at the same time our cells are literally starving.
If you can, paint a picture in your mind of a person sitting at a dinner table surrounded by food. Imagine that there is a gourmet meal prepared before this person. There is a wonderful salad, fresh whole-grain dinner rolls, stuffed pheasant hens, asparagus with a light cream sauce, and a decadent dessert of choice waiting for this person. However, for some reason, the person can not eat. The food is right there before them, but they can not open their mouths and eat it. Hunger consumes the person but there is nothing that they can do about it. This is what diabetes is like. There is plenty of food in the blood, however, the person can not utilize the nourishment provided for them.
Complications
When glucose levels in the blood remain too high for a period of time bad things happen. In the blood vessels, fat and other deposits, called arterial sclerosis or hardening of the arteries accelerates at an alarming rate. In fact, this problem is so bad, diabetes is one of the top risk factors of coronary heart disease, even above smoking. The relative risk for a diabetic to die from cardiovascular disease is 60- 70%, compared to 20-25% for non-diabetic. When this plaque gets in the small arteries of the eyes, blindness is often a rapidly following, irreversible result. This is referred to as “Diabetic Retinopathy”, which is the leading cause of blindness in the United States. In fact, up to 30% of those who develop diabetes as children will lose their vision later in life. Also, diabetes causes the red blood cells (which carry oxygen to the cell and carbon dioxide away from the cell, to lose their ability to release oxygen to the tissues for normal cellular
respiration. Lack of oxygen will lead to sickly tissue, which is most notable in the feet and ankles of long term diabetics.
The buildup of sugars in the fluid inside the eye causes the lens of the eye to become opaque, or to lose their transparency, leading to cataracts. We also find that when glucose levels are allowed to remain high, the insulation that surrounds our nerves (Schwann Cells) degenerate, which will eventually lead to a disruption of nerve communication. This is commonly called “Diabetic Neuropathy” which simply means that the diabetic’s ability to feel sensations is diminished or absent. Diabetic Neuropathy can assume a variety of forms. Most commonly, Diabetic Neuropathy affects the nerves of sensation of the legs. This becomes particularly alarming in light of diabetic foot ulcers and gangrene, which will be discussed momentarily. The problem arises because the person with Diabetic Neuropathy can not feel the sensations in the foot, so that when a painful event occurs, such as a thorn in the foot, a blister forming from new shoes or stepping on a sharp object the patient is not fully aware of the event and may do nothing to care for the feet. As well, when people who do not suffer from DM purchase a new pair of shoes, they generally look for a “fit” which they are used to. I purchase the shoes I do because I like the way they “feel” on my feet. I am looking for a particular “snugness” which I am used to and is comfortable. People suffering from Diabetic Neuropathy lose that ability, and consequently begin to purchase shoes of smaller and smaller size to get that same “feel”. Any of these events can lead to wound formation, which is often the initial insult which can result in diabetic foot ulcers and gangrene.
Diabetic foot ulcers are open wounds on the feet which are very resistant to healing. Many people with these ulcers carry them as open festering wounds for YEARS. The infection can get so bad that it invades the bones of the feet. The reason they develop are two fold. Diabetic Neuropathy as discussed above is one reason. The second has to do with the hardening of the arteries and the loss of the oxygen- carrying capability of the red blood cells. Because the arteries harden so rapidly, eventually they become clogged with the plaque, which decrease the volume of blood that can flow to the different parts of the body. Have you ever noticed when we get a cut or scrape, how the skin around the lesion turns red? This is because our blood vessels swell, rushing the infection-fighting substances in our blood to the injury to protect our body from infection. However, when the amount of blood flow to the legs has been reduced, often by more than 50% in the case of long standing DM, the ability of the body to deal with an insult is not there any longer. To compound matters severely, the blood that does arrive at the site may have a greatly lessened ability to provide much needed oxygen to the wound for healing. Oxygen is carried throughout our body by red blood cells. Diabetics have problems with the ability of their red blood cells to bind to oxygen and to then release it to the cells. This is why diabetic foot ulcers are such a concern.
Diabetic Nephropathy, or kidney failure, is the most common complication which leads to the death of the patient who suffers DM. The anatomy and physiology of the kidney is beyond the scope of this article, however it is noteworthy that the kidney functions to filter certain things (waste products) from the blood, while leaving beneficial things (blood cells, protein, glucose and minerals) in the blood. When kidney failure occurs, the ability of the kidney to filter is lost. Instead of filtering, the kidney allows all substances to pour through without selectivity. So, good things are lost, while waste products accumulate in the bloodstream, building rapidly to deadly levels .
TYPES OF DIABETES
In order to properly discuss diabetes, we must differentiate the types of diabetes. There are actually four types of diabetes. A brief explanation of each is given below:
1. Juvenile or Insulin-Dependent Diabetes Mellitus (IDDM). Generally patients who suffer this disorder are diagnosed as children. The cells which produce insulin in the pancreas, the beta cells in the Islets of Langerhans, are somehow destroyed. Theories on the cause of this destruction
vary, but include an autoimmune (where the immune system of the body actually attacks the pancreas believing that the pancreas itself is an infection) reaction to an insult such as viral infection, chemical injury or unknown toxin. This is the most serious form of the disease, and complications can rapidly threaten one’s life.
2. Adult or Non-Insulin Dependent Diabetes Mellitus (NIDDM). This is by far the most common form of DM, and is characterized by an impairment in the secretion of insulin. Eventually the amount of insulin secreted by the pancreas is insufficient to meet the needs of the body, and levels of blood sugar elevate. Other factors include a resistance to insulin at the cellular level. Insulin attaches to specific receptors (key holes) in cells. When resistance develops there can be a decrease in the absolute number of insulin receptors. In this event the actual amount of insulin in
the blood stream is higher than normal, however, it is ineffective and the patient still becomes hyperglycemic.
3. Gestational Diabetes. This is a hyperglycemic state which sometimes occurs during pregnancy. Very little is known about the cause of this form of diabetes, however, 50% of women who suffer from this disorder eventually develop Non-Insulin Dependent Diabetes Mellitus later in life. Because of this close association with the later development of NIDDM, causes and treatments in this work will consider Gestational Diabetes and NIDDM as the same problem. Complications from this disorder are different from other diabetes. The unborn child becomes the primary focus
of attention of physicians and unfortunately, the disease. Children born of diabetic mothers have a grossly increased frequency of birth defects. Their mothers suffer more often from toxemia of pregnancy, or very high blood pressure which can compromise the circulation to the unborn child (a cause for immediate delivery of the child). Children born of diabetic mothers are generally much larger than children born of mothers with normal blood sugar. This increase in size creates numerous problems upon delivery. Often the child is just too large to pass through the birth canal and emergency cesarean section is necessary.
4. Diabetes secondary to other causes. This can be caused by disorders such as tumors of the pancreas, infections of the pancreas and can occur as a reaction to some drugs. In these cases, the diabetic state is usually of a less concern than the problem that caused it.
DIAGNOSING DIABETES MELLITUS
Many of us know someone who returned from a visit to the doctor with a diagnosis of diabetic. But how does a physician diagnose diabetes? Most authorities use the National Diabetes Data Group of the National Institutes of Health guidelines for diagnosing diabetes:
1. Overnight fasting blood glucose concentration. This is when the patient is told not to eat anything after midnight. Then in the morning the laboratory draws the patient’s blood and measures the amount of glucose in the blood. If the glucose is more than or equal to 140 mg/dl on at least two separate occasions (with normal being in the range of 70- 110) the patient is diagnosed as having diabetes.
2. Glucose Tolerance Test: Following ingestion of 75 grams of glucose (or 300 calories of pure sugars) blood glucose concentration greater than or equal to 200 mg/dl two hours after ingestion.
A third method that is generally reliable is the random finger stick. This is the common at home variety of blood glucose monitoring. People can purchase these machines from their local drug or discount store, prick their own finger, and have the machine read the level of glucose in the blood in the privacy of their own home. When there are two separate, random readings above 140 but below 200 it is generally diagnostic of diabetes. While a single reading above 200 is diagnostic of at least having glucose intolerance, if not full blown diabetes. Patients with random levels above 350-400 may not even know that they are diabetic! The disease silently erodes their body but they have no idea!
An older method of detecting DM is to monitor the urine for “spillage” of glucose. As was mentioned above, at times when the level of glucose in the blood remains too high, the kidney will fail to be able to filter it out and the glucose will “spill” into the urine. A “dipstick” with chemically sensitive strips is placed into a cup of urine, and the level of glucose is measured by the color change on the chemical strips. Generally, if one does not spill sugar, the strip will remain white to blue-gray, while the most extreme cases of spilling glucose will turn the strip brown.
As well, physicians look for what is referred to as the classic triad of symptoms of diabetes which include: polyuria, which is frequent urination; polydipsia, or frequent thirst; and polyphagia, or increased hunger (generally only associated with Type I DM).
NUTRITIONAL AND ENVIRONMENTAL FACTORS CAUSING DIABETES
Once again, it will be important to differentiate Insulin and Non-Insulin Dependant Diabetes Mellitus. Research on the causes of IDDM is seriously lacking, however, there is some evidence which points to some nutritional and environmental factors. As was mentioned, IDDM is characterized by destruction of the beta cells of the Islet of Langerhans in the pancreas. But what causes this destruction? Some evidence has suggested that some nutritional factors play a role. There is a chemical called Streptozotocin, which is a derivative of the amino acid glucosamine and is found in smoked meats. This same chemical synthetically produced is the toxin of choice for laboratory experiments which destroy the beta cells in animals to experiment on diabetes. It is administered to the animals in order to induce IDDM.10 There has also been shown to be a correlation between the consumption of whole cow’s milk and IDDM. Perhaps the strongest theories surround a viral origin of the beta cell destruction. A brief explanation of virology is necessary here. Viruses can not live outside of a “host” cell, while bacteria can live on the kitchen counter for several hours, and many can even flourish. Viruses depend on a host cell for all its needs. A virus will enter a host cell and live on the host cell’s food sources. The virus will use the host cells different organisms to reproduce itself over and over again until the host cell becomes so full of the virus that the cell wall blows up, thus killing the host cell and releasing millions of other viruses who now need to find a host cell of their own. We have all suffered from the common cold. This is a virus which likes to live in the respiratory tract. It will not live in the stomach, it will not live in the liver, it will not live in the pancreas. Research has suggested that there is a viral element to IDDM, which can destroy the beta cells.
There is much more research which suggests nutritional factors in the cause of Non-Insulin Dependant Diabetes Mellitus, which is by far the most common form of the disease. It is important to note that diabetes occurs rarely in countries which do not consume the traditional Western diet. Africans, Asians and Polynesians whose diet consists primarily of vegetables, whole grains and other starches and fruits generally do not develop diabetes. However, if we take these people and move them to a Western country and feed them a Western diet diabetes, as well as other Western illnesses such as heart disease and cancer will approach levels found by the native people of their new Western country. I know that many of you are not convinced, however, you soon will be. Micronesia is a group of islands in the Pacific, east of the Philippines. One of the Micronesian islands, Nauru, was inhabited by a group of natives for hundreds of years. These people led a quiet life, eating traditional Polynesian foods including taro (a potato like starch), breadfruit, coconuts, native fruits and vegetables and fresh fish. Naturally, their health was excellent. Degenerative diseases were practically unheard of. However, during World War II, it was discovered that this island was a rich source of phosphates, a commodity the West was eager to purchase. As a result, the people of Nauru became some of the richest people in the world. They no longer had to rely on the land and sea and their natural sources for food. The people of Nauru were able to import the rich foods of the world. Canned foods, frozen dinners, soft drinks, oils, white flours and bakery items became their mainstay. So rich was their new diet that it was not uncommon for a Nauruan to have two or three different kinds of meats at one meal. As a result, their intake of dietary fat skyrocketed, while fresh fruits and vegetables, with their nutrients and fiber decreased dramatically. As a result of this decadence, diabetes has become a crisis to this island nation with 34.4% of the population over the age of 15 having diabetes. That is more than 1/3 the adult population!!! Where did the problem come from?
THEIR DIET!!!
Other research has clearly demonstrated that a diet high in fat can cause diabetes. As far back as 1927 diet was suspected in the onset of diabetes and a physician named Dr. S. Sweeney took some of his medical students and placed them on a diet consisting of olive oil, butter, mayonnaise and 20% cream for a period of two days. Following this two day gluttony, the students were given a glucose tolerance test. The results? ALL STUDENTS BECAME DIABETIC!!! Their blood sugar levels were clearly in the diabetic range, some in the critical range. Later, Dr. Sweeny placed the same students on a two day diet of simple and complex carbohydrates, including traditionally taboo items like sugar, candy, pastry, white bread, syrup, and other complex carbohydrates like rice, fruit, oatmeal and potatoes. The results? All students’ blood sugar levels were in the normal range.
What we can conclude from Dr. Sweeney’s experiments is that ONE way diabetes can be caused is the consumption of a diet high in dietary fat. Carbohydrates, which are broken down into glucose, have for years been thought of as causing diabetes. In fact, the term Sugar Diabetes was used for years to label this disease. However, carbohydrates can actually make insulin more effective in the body of the diabetic. In one research project, a group of people suffering from adult onset diabetes were taken and placed on a diet consisting of 85% sugars coming from high carbohydrate foods and simple sugars. During the study these people’s blood sugar levels actually decreased in spite of the levels of sugar in the diet.
Another undisputed factor in the development of diabetes in the adult population is obesity. One reason is that as a person’s weight grows it becomes harder and harder
or the insulin to reach the cells of the body. As one grows larger, the amount of blood in the system, because of size alone, can actually double. Also, an obese person generally consumes a much higher caloric intake, (much of which is fat calories,) than one who is lean. This puts double the amount of work on the pancreas. This overworking of the pancreas can lead to insulin insensitivity, or when there is insulin in the body either the insulin is of a poor quality or the receptors on the cells do not recognize the insulin. Dr. John Butterfield, Professor of Medicine at Guys Hospital in London, believes that when fat competes against muscle for insulin, the fat cells usually win, thus exacerbating the problem for the obese person. However, it has been shown that weight loss, particularly referring to the amount of fat carried by the body, improves the diabetic’s condition and may in itself lead to a disappearance of diabetic symptoms. Deficiencies in certain vitamins and minerals have been shown to have a negative effect on the diabetic’s condition and may be contributory to the development of certain types of diabetes. A deficiency in a little talked about trace mineral, called Chromium, has been shown to contribute
to the glucose intolerance exhibited by people suffering from diabetes. Chromium is used either in the production of insulin in the pancreas, or at the cell’s receptor site. In either case, chromium exerts its effect by allowing insulin to attach to the receptor site of the cell and cause glucose to
enter the cell. Studies by Dr. Walter Merz while the chief of the USDA’s Vitamin and Mineral Research Division have concluded that chromium deficiencies can actually cause diabetes.
Another dietary deficiency which is rampant in our Western diet and particularly notable in the onset of diabetes is the lack of dietary fiber. Fiber has many actions in the digestive system. Of concern to the diabetic, dietary fiber acts to slow absorption of digested food in the intestinal system. Because of this slowing, there is not a rush of digested food products into the bloodstream, and the body is more able to handle the load.
DIABETIC PHARMACOLOGICAL THERAPY
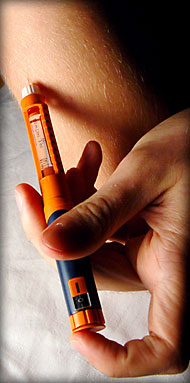
The insulin dependant diabetic will obviously require multiple daily injections of insulin in order to stay alive. The insulin that is used was once extracts from either hogs or cows pancreases during slaughter. Today synthetic insulin is available, both in long term and short acting varieties. The problem that arises with insulin therapy is that after some twenty years of taking the drug, the body may begin to become hypersensitive to it and reject it. Physicians usually do not discuss this with their patients who may have no warning prior to the insulin not doing its work in their body. A second and more severe complication with the use of insulin is referred to as ‘an insulin reaction’. This is when the levels of blood sugar become very low and the person will have an induced HYPOglycemia. Because long acting insulin can continue to reduce blood glucose levels for 6-12 hours, during an insulin reaction a diabetics blood sugar level can become so low that they can lapse into a coma, and death can even ensue. Actually, the most dangerous complication of diabetes is this insulin reaction.
By far the most common form of diabetic pharmacological treatment are drugs called “sulfonylureas”. These are prescribed for the non insulin dependant diabetic. These medications act by stimulating the pancreas to secrete more insulin that it would otherwise. These drugs can also cause hypoglycemia as in the insulin reaction, however, that is not my largest concern. Investigators reported in 1970 that a study with over 800 diabetics demonstrated that people who took these drugs to control their blood glucose MORE THAN DOUBLED THEIR RISK OF DEATH FROM HEART ATTACKS!!! As we mentioned earlier, diabetes in itself increases the risk of heart disease and rapidly increases the progression of atherosclerosis (hardening of the arteries with plaque), but people taking the oral diabetic medications HAVE MORE THAN TWICE THE RISK OF HEART ATTACK AS DIABETICS NOT TAKING ANY MEDICATIONS AT ALL!!! Though many physicians do not discuss this risk with their patients, the risk is clearly written on the insert of the prescription bottle.
| ***A Word Of Warning*** |
| We DO NOT recommend to anyone on any prescribed medication to discontinue taking their medications without the advise of their physician. Our recommendation is to implement the program we will outline below and under the guidance of a qualified physician then to decrease and perhaps eventually eliminate the need for medications. Changes in medications should only be initiated on the advice of a qualified medical health professional. One point must be fully explained at this point. The Type 1, Insulin Dependant Diabetic, according to current medical understanding, will necessarily require insulin injections or supplementation for life. The information provided below is designed for the Adult Onset, or Non-Insulin Dependant Diabetic patient, and the belief that diabetes can be reversed by diet and nutritional means is specifically intended for patients in this (NIDDM) category. However, the Insulin Dependant Diabetic can greatly benefit from the advice described below. I believe that the IDDM patient will improve their quality of life, reduce the risk of complications and perhaps even reduce their need for insulin injections if they follow these guidelines. But again, begin no change in your diabetic treatment without the advice of a qualified physician who is familiar with your personal medical history. |
TREATING DIABETES NATURALLY
Diet therapy is the first line of defense in the battle against diabetes. Usually when a person is diagnosed as having diabetes, their physician gives them some information on the American Diabetic Association and American Dietetic Association (ADA) Exchange Diet. This is a diet program based upon an exchange principle. A person on this diet is allowed a number of “Exchanges” or foods from specified groups. There are six groups of food in this plan: Milk, Vegetables, Fruit, Bread, Meat and Fat. Basically, when one is placed on a 1,800 calorie a day diet, they would be allowed 2 Milk Exchanges, 3 Vegetable Exchanges, 5 Fruit Exchanges, 9 Bread Exchanges, 7 Meat Exchanges, and 5 Fat Exchanges. See Table 1 for more information.
Table 1. ADA Exchange Diet Basic Composition Per Serving or Exchange*
EXCHANGE CALORIES CARBS(g) FAT(g) PROTEIN(g)
Milk 170 12 10 8
Vegetables 35 7 --- 2
Fruit 40 10 --- ---
Bread 70 15 0-.5 2
Meat 75 --- 5 7
Fat 45 --- 5 ---
* The ADA Diet was designed and regulated by the American Diabetic Association and the American Dietetic Association. The exchange diet is copywright by these organizations. In order for the above chart to really make sense it is necessary to understand just how much an exchange is for each food type.
Milk: 1 cup sugar free yogurt, 1 cup whole milk. Vegetables: 1 cup cooked broccoli, 2 cups asparagus, 1/2 cup cooked carrots. Peas and corn are not recommended. Fruit: 1/2 banana, 3/4 cup fresh pineapple, 1 orange, 1 large apple. Bread: 1 slice of whole wheat, white or rye bread, 1 English muffin or 1 bagel. Meat: 1 oz. roast beef, 1 oz. fresh fish, 1 oz. chicken or 1
egg (limit to 3 eggs per week). Fat: 1 tsp. mayonnaise, 1 tsp. butter.
The major emphasis of the ADA diet is to restrict caloric intake, thus, hopefully reducing the diabetic’s weight. Losing weight makes the body’s cells more responsive to the insulin that is produced. Thus, weight loss alone can produce a “cure” for many new onset diabetes.33 However, I believe that the ADA diet is problematic in several ways. First and foremost, the ADA diet allows for daily fat consumption (from milk, meats and fat categories) to be up to 35% of total caloric intake. This is way too high. As we saw with Dr. Sweeney’s research, high fat intake can induce the diabetic condition. The ADA diet also recommends that saturated fat intake be one-third total fat intake, and to limit cholesterol to less than 300 mg/day. However, they make no mention of hydrogenated fats and oils, which though contain no cholesterol in themselves, can actually cause the body to produce more cholesterol, thus increasing one’s blood cholesterol
level.
Carbohydrates consist of 40-50% percent of daily caloric intake in this diet, a figure I consider much too low, while meats make up the rest of the daily food intake. The Exchange Diet also limits vegetable consumption to 3 servings a day, with only 2 of those servings being raw. I really cannot see the sense in this. Fresh vegetables are packed with vitamins, minerals and fiber. To limit their consumption is ridiculous.
The EAT DRINK AND BE HEALTHY DIET PROGRAMis a diet program that is high in carbohydrate, low in protein and fats, and high in dietary fiber. This diet program has taken into account much of the research conducted by numerous scientists, who found that such diets actually reduce the diabetic’s hyperglycemia, complications and in many cases reverse the disease process. I recommend that the diet consist of 70-75% complex carbohydrates, 15-20% proteins, and only 10-15% fat, and that the fat be non-hydrogenated and unsaturated or poly unsaturated. The EDBH Diet utilizes high-carbohydrate food sources which are high in natural plant fiber. Whole beans, brown rice and whole grains are the cornerstones of this program. Please refer to our cookbook for excellent recipes.
SPECIFIC NUTRIENT THERAPY
Deficiencies in several nutrients have been shown to increase the incidence of diabetes, and scientific research has demonstrated that supplementation with the specific nutrients described below can greatly improve the diabetic’s condition. In fact, evidence is mounting that supplementation with the antioxidant group of vitamins, combined with yeast-chromium, magnesium, zinc, pyridoxine and gammalinolenic acids actually improve glucose tolerance, stimulate immune defenses, promote wound healing, while reducing the relative risks from the complications of diabetes.38
BENFOTIAMINE (Health Masters’ B Complex) is a fat-soluble form of vitamin B1 (thiamine) and is the most effective metabolic precursor of active thiamine, or vitamin B1, available. It also supports healthy blood sugar metabolism. Thiamine is water-soluble, which makes it less available to the interior of the cell. The difference here is that benfotiamine can easily penetrate into the inside of cells and is more bioavailable than the water-soluble thiamine.
CINNAMON (Health Masters' Cinnamon Extract Fuel Burner) adds a 'supercharged' extract of 100% safe and effective therapeutic blend of cinnamon, chromium and other powerhouse nutrients to reduce blood glucose, triglycerides, LDL cholesterol and total cholesterol in people with type 2 diabetes. Cinnamon has long been recognized for it's ability to help the body's conversion of sugar (glucose) into energy. Studies show including cinnamon in the diet of type 2 diabetics will reduce risk factors associated with diabetes and cardiovascular diseases.
BIOTIN (Health Masters' Ultimate Multiple Vitamin) Biotin is one of the lesser known B vitamins. It is normally found in meats, dairy products and whole grain cereals. It is not on the Food and Drug Administration’s US Recommended Daily Allowance (U.S.RDA) list, however it is a vital micronutrient. Biotin is not normally supplemented by most over the counter vitamins or by food replacements for dieters of people who are too ill to eat for themselves. The Journal of Parenteral & Enteral Nutrition reported that hospital patients receiving intravenous (IV) feedings without biotin suffered a variety of symptoms including depression, nausea and lethargy. Supplementation with 300 micrograms of biotin relieved symptoms in only 5 days.39 The Annals of the New York Academy of Science reported a study where patients with Insulin-Dependant Diabetes Mellitus were taken off their insulin therapy and given either 16 milligrams of biotin or a placebo for one week. The results were very encouraging. The fasting blood glucose levels of the placebo group rose dramatically, as would be expected with a person who has diabetes. But the group who received the biotin therapy actually had their blood glucose levels FALL significantly.
VITAMIN C (Health Masters' Excellent C) Experimental studies have shown that diabetic patients excrete more ascorbic acid (vitamin C) in their urine than do non-diabetics.40 This is also associated with the increase in atherosclerosis in diabetic patients.41 Diabetic patients receiving 500 mg vitamin C supplementation twice daily demonstrated improved glucose tolerance tests IN JUST TEN DAYS!!! Supplementation has also shown to reduce serum cholesterol and triglycerides. As little as 500 mg daily can have dramatic effects. In one study patients received 500 mg vitamin C for one year. After that time the patients experienced AT LEAST 40% reduction in serum cholesterol and a significant reduction in triglycerides.
NIACIN (Health Masters' Vascular Relaxant) Niacin is one of the elements in the energy transfer system of the body. Niacin is involved in the body’s utilization of glucose, the body’s tolerance of glucose. Thus a deficiency of niacin will interfere with the utilization of glucose and energy production.
VITAMIN E (Health Masters' Vitamin E) Studies have shown that vitamin E may reduce the insulin requirement of diabetics dramatically. Further, diabetics on insulin therapy should begin vitamin E therapy with 100 I.U. daily, monitor their blood glucose levels AT LEAST four times a day, and do so only with the cooperation of a qualified medical person.
Diabetic patients have an increased requirement for vitamin E, as well, deficiencies of vitamin E may promote the cellular and vascular damage associated with diabetes (as well as other conditions).46,47 Supplementation has proven very beneficial. Numerous studies have shown that supplementation with vitamin E often improves the diabetic’s condition as well as reduce the complications of the disease, especially those associated with the vascular system and skin ulcers. In a case reported in Clinical Medicine, a diabetic patient with a large, yellow ulcerating lesion on the leg was administered 150 mg vitamin E through injection twice a week, and 100 mg orally three times a day. In just TWO WEEKS the ulcers were closed and normal skin formation began.!!! A second report in the same journal discussed a woman who had suffered three lesions on her leg for over one year. This woman was given the same treatment, however, her results were not as rapid as the first. This time it took THREE WEEKS for the ulcers to heal!
COPPER Copper is one of the micronutrients we hear very little of. A micronutrient is a vitamin or mineral which the body needs very small amounts to suffice its needs, and too much will actually be toxic to the body. Generally the body’s needs are met through diet. However, deficiencies in copper is associated with glucose intolerance. Excess intake of micronutrients can be toxic, therefore, supplementation should be limited to 2 mg daily, or equivalent to the
US FDA Recommended Daily Allowance.
MANGANESE (Health Masters' Ultimate Multiple Vitamin) It has been clinically demonstrated that manganese levels in diabetics are one half that of normal, healthy individuals.50 In animal studies, guinea pigs fed a diet deficient in manganese became hyperglycemic. Even more alarming is the fact that the offspring of these guinea pigs were born with abnormalities of the pancreas. In one study of manganese supplementation, a 21 year old insulin dependant diabetic was given 3-5 mg manganese daily. His
results were dramatic, experiencing a consistent fall in blood glucose levels, often actually becoming severely hypoglycemic. Others in the study did not have such dramatic results, suggesting that results are dependant on individual manganese levels.
PHOSPHORUS (Health Masters' GHI Cleanse) Deficiencies of phosphorus have been demonstrated to impair the ability of insulin to regulate blood glucose. Phosphorus deficiencies are also associated with some of the vascular complications of diabetes. A substance called 2,3-diphosphoglycerate is a molecule found in our blood which regulates the way oxygen is released from the red blood cells to the cells for normal gas exchange. As the name implies, phosphate is the main component of this molecule, and shortages of phosphate in the system will lead to imbalances, which can lead to problems including poor oxygenation of tissues which is associated with diabetic foot ulcers and other vascular abnormalities. Supplementation with 2 grams, 3 times a day has demonstrated improvement with the oxygen carrying capacity of the red blood cells, and patients receiving this treatment felt less tired. As well, control of their blood glucose levels vastly improved. Further, after two years of supplementation, the patients in this study showed no evidence of adverse effects from the large dose of phosphorus supplementation.
POTASSIUM (Health Masters' GHI Cleanse) Potassium deficiency has been clinically shown to cause a decrease in insulin levels and increases in the resistance of the insulin receptors. Supplementation of potassium was associated with significantly higher insulin levels and improvement of glucose utilization.
ZINC (Health Masters' Zinc Glycinate) Diabetics tend to hyperexcrete zinc through their urine, even when kidney function is normal according to laboratory tests. Further, the degree of excretion of zinc is correlated with level of glucose in the urine. In clinical tests, non-diabetic subjects were alternately fed a diet with insufficient zinc, then a diet with zinc supplementation. What was interesting is that the levels of zinc in the blood stream remained fairly constant, regardless of the amount of zinc in
the diet. However, when the subjects were on the low zinc diet, their blood glucose significantly increased, as well as the amount of fats in the blood (which could later be laid down in the arterial walls).
COENZYME Q10 (Health Masters' CoQ10 ) Coenzyme Q10 (CoQ10), also known as ubiquinone is a little known nutrient. It is an essential component of the mitochondria, or the organelle which produces cellular energy. CoQ10 can be synthesized in the body, but deficiencies have been reported. In observational studies, diabetic patients tend to have deficiencies in CoQ10 almost ten times as often as non-diabetics. In fact, as many as 20% of diabetics receiving oral hypoglycemic drugs were deficient. (This can have severe cardiovascular effects. See the Feb 95 issue of EDBH!) Supplementation has proven quite beneficial for all diabetics. A group of 39 diabetics were given supplementation for a trial ranging from 2 to 39 weeks. The results were astounding, with many experiencing as much as a 30% drop in fasting blood sugar.
SPECIFIC NUTRIENT THERAPY FOR
SPECIFIC COMPLICATIONS OF DIABETES MELLITUS
As well as the nutrients listed above, some experiments have demonstrated that specific nutrient therapy could reduce if not reverse some of the complications of diabetes not already listed above. Patients suffering from Diabetic Neuropathy have been shown to have a deficiency in Pyridoxine, or vitamin B6. One study demonstrated that in patients symptoms of Diabetic Neuropathy supplementation with vitamin B6, 50 mg three times daily brought about an improvement in symptoms in just 10 days!! Further, these patients condition continued to improve, and actually symptoms disappeared in many patients!! Vitamin B6 has also proven
beneficial in pregnant women suffering from gestational diabetes. In one study, 14 pregnant women who had sufficiently abnormal glucose tolerance tests to be diagnosed as having gestational diabetes were given 100 mg vitamin B6 daily for two weeks. After this time, all but 2 of the women’s blood glucose levels were within normal limits. Thiamine supplementation has been shown to improve the sensory system, or the ability to feel. Stanley Mirsky, M.D., President of the New York affiliate of the American Diabetes Association wrote that during his clinical experience, as much as 80% of patients experiencing Diabetic Neuropathy experienced a dramatic improvement in symptoms with 100 mg thiamine daily IN JUST TWO WEEKS!!!
MAGNESIUM (Health Masters' Magnesium Glycinate) has been shown to be particularly deficient in diabetics, especially those suffering from diabetic retinopathy. The decrease of magnesium in the blood is associated with elevations of the substances which lead to atherosclerosis and hypertension (high blood pressure). High levels of magnesium in the blood are associated with decreasing elevations of the substances which cause atherosclerosis and hypertension. Recall that blocking of the arteries
to the eyes is one of the causes of diabetic retinopathy. Supplementation with magnesium helps prevent the blocking of the arteries to the eyes and can offer protection against diabetic retinopathy.
FATTY ACIDS (Health Masters' Norwegian Omega 3) In the 90’s fat is a taboo word. However, there are actually “good fats” which we unfortunately do not have much of in our Western diet. These fats, called Omega-3 and Omega-6 fatty acids because of their molecular structure are found in plant (Omega-6) and fish (Omega-3) sources. The supplementation with fatty acids have proven extremely beneficial in many cases of diabetes. Omega-3 fatty acids have been shown to decrease insulin resistance in NIDDM. Omega-6 fatty acids have proven to have a cardio-protective dimension. In one study, 102 newly diagnosed diabetic patients were placed on the normal Western diet. Half the group received supplementation with Linoleic acid (an Omega-6 fatty acid source), while the second half received no supplementation. After 5 years, none of the supplementation group had died from heart attack, while three of the non-supplementation group had died. Of the survivors, only 6% of the males and 4% of the females who had received supplementation had any signs of cardiac ischemia, while 22% of the males and 16% of the females who did not receive supplementation had signs and symptoms of ischemia.
EXERCISE One of the most neglected tools in the battle against diabetes is exercise. Daily exercise will benefit the diabetic patient in several ways. It will reduce body fat, which will reduce the need for insulin. Exercise will also make the insulin that the body produces more effective in its job. Exercise will reduce the cardiovascular complications associated with diabetes.
Once again, a word of warning must be given. Do not begin an exercise program without the advice of a qualified physician. The main reason we state this is that diabetic patients come in all shapes, sizes and ages, with different exercise tolerances. A elderly woman who has been suffering the ravaging effects of diabetes for 40 years will not have the exercise tolerance that a man of 45 who is just diagnosed with diabetes will have.
I recommend that all diabetic patients find their exercise tolerance, and work to 60-80% of that tolerance, for a minimum of 30 minutes a day, six days a week. For some, this may mean doing range of motion training in a swimming pool. For others, walking or even jogging may be instituted from the beginning of their program. We have just completed a new video series on aerobic exercise which is available by calling our office. The most important aspect, other than working with your physician, is consistency. Exercise will lower blood sugar levels, but permanent changes require time. Remember, the adult onset diabetic did not develop the disease overnight, and it may take a few weeks to see a dramatic difference in the area of exercise.
SPECIFIC NUTRITIONAL RECOMMENDATIONS
KEEP YOUR FAT INTAKE TO 10-15% OF DAILY CALORIE INTAKE. You can measure this by taking your total calorie intake, say 1800 calories, and divide by 10 which gives 180. Each gram of fat contains 9 calories, which means that on the 1800 calorie diet, a person could consume 180 calories, or 20 grams of fat. NO DAIRY PRODUCTS. All dairy products must be eliminated. This includes milk, cheese, ice cream and yogurt. NO JUNK FOOD. If it comes in a cellophane wrapper throw it away. NO FRUIT JUICES. Fruit juice is a very concentrated source of sugar and sometimes can contain more sugars than soda. Eat the fruit instead. It has more fiber and vitamins. NO HYDROGENATED OILS. This means margarine, Crisco, and the thousands of products, like Jiff peanut butter which contain them. READ THE LABEL!!! If the ingredients say hydrogenated, partly hydrogenated oil, or pure vegetable shortening, LEAVE IT ON THE SHELF!!! Use olive or canola oil for your oil needs. However, use these products sparingly because they are 100% fat. ELIMINATE SUGAR INTAKE.
Once again, read the labels and get it out of the diet! ELIMINATE CHOCOLATE AND OTHER CANDY. Also, eliminate any source of caffeine. NO NUTRASWEET PRODUCTS. Instead, try Barley Malt Sweetener, which is available at all quality health food stores. It is not very expensive, and is an all natural product. Aspartame interferes with the blood sugar regulation in your body. Researchers have theorized that use of aspartame can cause people to actually gain weight. Plus, Aspartame, because of its methanol content it is extremely toxic. Watch for an upcoming issue of the EAT DRINK AND BE HEALTHY newsletter on NutraSweet! NO MONO-SODIUM-GLUTAMATE OR MSG. Besides being loaded with excess sodium, MSG damages brain cells along with its cousin NutraSweet (both are called excitotoxins in neurochemistry.) NO PROCESSED MEATS. This includes most meats purchased in the deli case. Also, if it has Sodium Nitrate leave it alone. NEVER EAT PORK OR SHELLFISH. NO MAYONNAISE, which is usually 100% fat. EAT FRESH FRUIT AND VEGETABLES AS MUCH AS POSSIBLE!!! NO ALCOHOL. Just one ounce of alcohol can decrease the body’s ability to burn fat by up to 35%.
USE THESE HEALTH MASTERS' SPECIFIC VITAMIN SUPPLEMENTS |
| INSULIN SUPPORT -This product contains chromium picolinate and vanadyl sulfate. These elements enhance the metabolic effects of the body’s own insulin and promote glucose transport across the cell membrane, making cellular energy transfer more efficient. They can also reduce sugar cravings. Take 1 capsule twice daily. |
| OSSOMAG - Calcium/Magnesium - take 2 capsules twice daily. |
| COQ10 – take 2 capsules twice daily |
| ZINC GLYCINATE -1 capsule twice daily (40 mg daily) |
| FLAX SEED OIL - 4,000 mg daily |
| PRIMROSE OIL - 2,000 mg daily |
| SUPER POTENT E - 2 softgels daily (800 IU daily) |
| HGH STIMULATE -1 packet twice daily |
|
CINNAMON EXTRACT FUEL BURNER -2 capsules twice daily B COMPLEX - 4 capsules in AM |
Also, I get asked alot what is the best if I can only buy one thing for blood sugar on a small budget. For that I recommend the Glucose Buster, you can also read that artilce here.





